medical 3d printing, is always grinding deeply and vertically in last 2-3 decades
Note: This article is organized and expanded based on the video content of Bilibili creator “Owen 来造” (Owen to Make), presented from a third-person perspective. All images in the article are sourced from their video.
3D Printing is Transforming the Traditional Rehabilitation Orthotics Industry
Early applications of 3D printing in medicine were largely limited to supportive applications such as surgical guides and medical models. Subsequently, the technology gradually moved into more clinically integrated scenarios, including customized orthopedic implants and dental aligners. Today, 3D printing is even extending into the bioprinting of skin, cartilage, blood vessels, and even organs.

Yet on the other side, a huge market has long remained in the “handmade era”—the rehabilitation orthotics industry.
This industry is not small, nor is demand weak, but it has consistently lacked meaningful manufacturing upgrades. Only as 3D printing begins to enter the field are signs of change finally emerging in this traditional and fragmented niche sector.
Rehabilitation orthotics are essentially external support devices worn on the limbs or torso, primarily used for protection, support, and correction. They are widely applied in scenarios such as scoliosis, fracture fixation, and stroke rehabilitation, and represent a non-surgical treatment option that many patients cannot avoid.

Among these applications, scoliosis is perhaps the best entry point for understanding the industry’s problems and observing technological change.
Next, let’s take scoliosis orthotics as an example to see how 3D printing is reshaping the rehabilitation orthotics industry.
An Undervalued Market of Essential Demand
Many people may not realize that scoliosis is rapidly becoming a seriously undervalued market of essential demand.
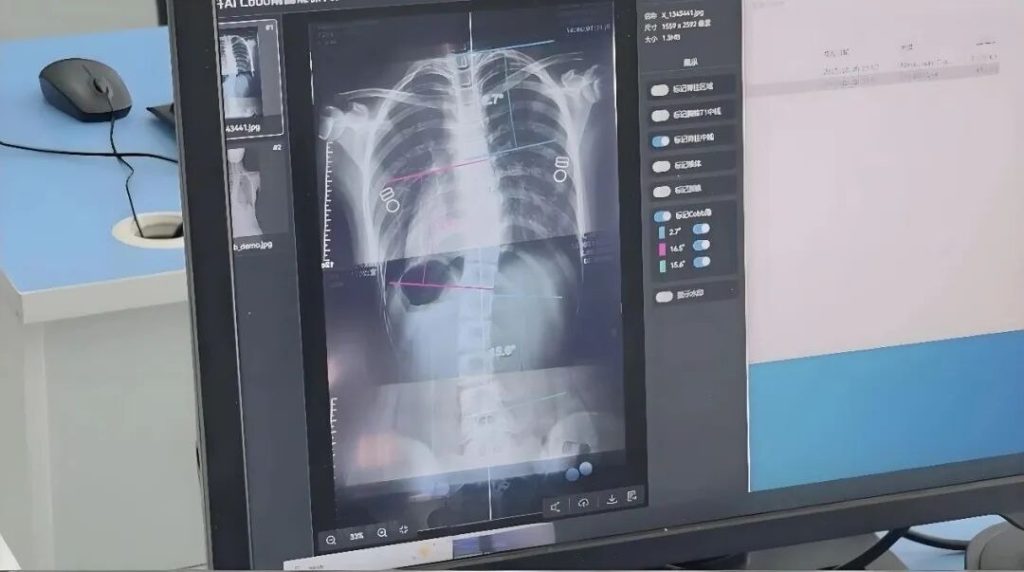
In China, scoliosis has become the third-largest threat to teenagers’ health, following obesity and myopia. Public data shows that the number of affected primary and secondary school students has exceeded 5 million, with the population continuing to grow by approximately 300,000 each year. But more critically, only about 10% of these patients actually require surgery. The remaining 90% all point to the same solution—orthotic bracing.
This is a “slow business”—requiring 18 to 23 hours of daily wear, lasting months or even years. For this reason, factors such as comfort, weight, breathability, and appearance—which may seem like mere experiential elements—actually directly determine patient compliance and, consequently, whether the treatment is effective.
A Typical “Handycraft Industry”
Demand is high, but the supply side remains quite primitive. Even today, orthotic manufacturing still carries distinct “handicraft industry” characteristics.

The most traditional method is plaster casting. A negative mold is made by wrapping plaster bandages around the patient’s body, then a positive mold is created from it. Technicians manually shape the positive mold, and finally, a heated plastic sheet is vacuum-formed over it. However, behind this seemingly mature process lies a heavy reliance on the experience of skilled labor, making standardization difficult. Moreover, the more steps involved, the more pronounced the accumulation of errors becomes.

The process is also not very patient-friendly.
It often requires standing still for long periods, with the mold-taking process feeling stuffy and causing noticeable pressure. The resulting orthotic devices are heavy, lack breathability, and are far from aesthetically pleasing.

The production side also faces significant bottlenecks. A skilled technician can produce at most 2 to 3 units per day. During peak seasons, the only way to increase capacity is by “adding more people.”
This is why the plaster-based process is being gradually phased out, and now remains primarily in regions with lower levels of digitalization.
Semi-Digitalization: Only Solved Half the Problem
The industry has not been without progress.

The current mainstream solution has already been upgraded to “3D scanning + CNC carving.”
The process appears more modern: the patient’s body is scanned, the data is combined with X-ray modeling, and analysis and modification are completed in software. A foam positive mold is then carved using CNC equipment. Compared to manual sanding and crafting, this step indeed relies more on data and is more consistent.
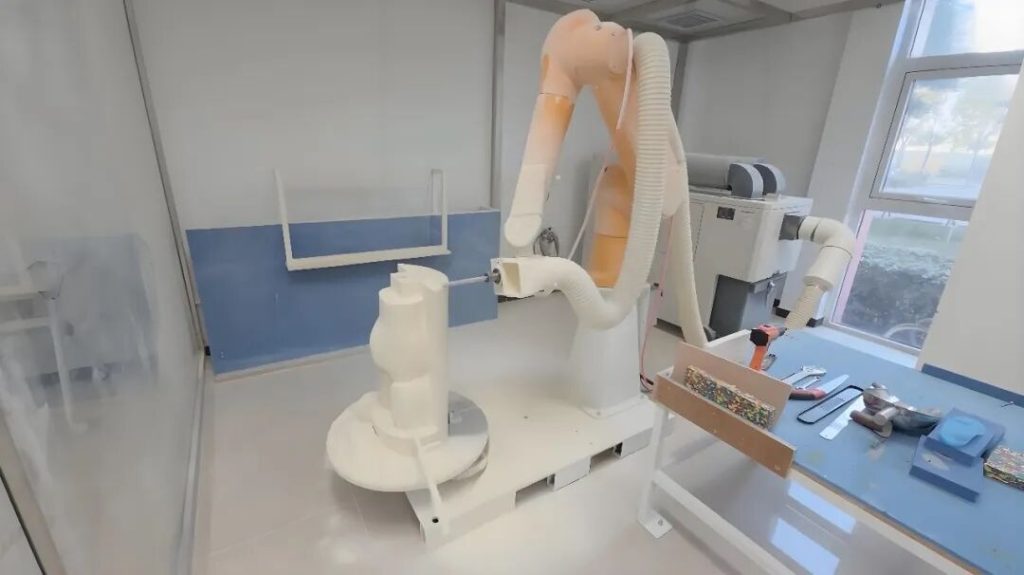
However the point is that this is only half digitalization

At the back end, the process still reverts to the old way. Heated PP or PE sheets are still formed over the positive mold, followed by trimming, sanding, and assembly before the orthotic device is finally completed.
The mold remains. Manual labor remains. The errors also remain.

In other words, whether using plaster casting or CNC carving, traditional orthotic manufacturing cannot avoid the positive mold step. It takes up space, generates waste, and requires troublesome post-processing. More critically, this model has never been able to escape the old problems of traditional manufacturing: low efficiency, over-reliance on experience, and difficulty in being replicated and scaled.
3D Printing Doesn’t Just Change the “Final Step”
Many people assume that 3D printing simply replaces the step of “making the orthotic device.”
But the real change actually happens much earlier in the process.
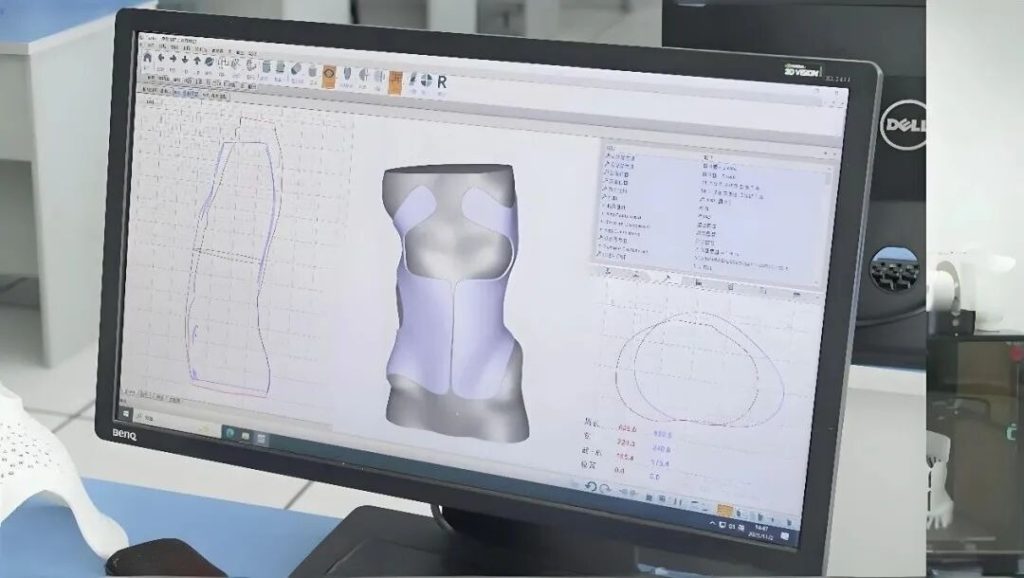
A more typical new workflow is taking shape: first, obtain body data through 3D scanning, then perform digital modeling and orthotic design, and finally print the device directly.
The most fundamental change behind this is that orthotic design is shifting from relying on a technician’s “feel-based shaping” to data-driven digital design.

This is precisely where the value of 3D printing lies. It doesn’t just change the manufacturing method; more importantly, it enables the precise translation of digital design outcomes into physical objects—including the orthotic’s shape, force distribution, and pressure point placement.
This is something unattainable with traditional craftsmanship.
In fact, traditional orthotics are essentially the processing of a single plastic sheet. 3D printing, by contrast, transforms the orthotic into a structural design.
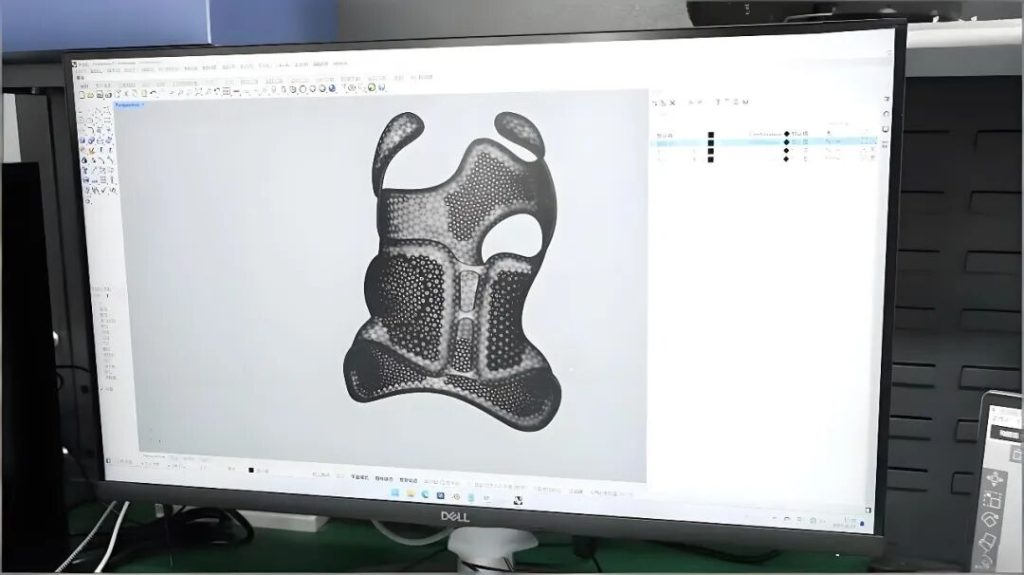
For example, large-area hollowing can improve breathability, local thickening and reinforcing ribs can enhance structural support, and personalized patterns can be added to increase acceptance among pediatric patients. When combined with simulation technology, it is even possible to identify and optimize pressure points to prevent discomfort before the device is ever manufactured.
From “Manual Customization” to “Mass Customization”
Another easily overlooked change is scale.
The problem with traditional orthotics is not just that they are slow to produce, but more fundamentally, the process remains a form of manual craftsmanship. It can be customized, but it is difficult to replicate; it can serve an individual, but it is hard to achieve scale.

This is precisely what 3D printing changes. Once the design is completed, the subsequent production can be largely handed over to the machines. As long as the number of machines can keep up, the production capacity can theoretically be scaled up indefinitely.
In many cases, the manual operation time—from data processing and material preparation to machine setup—takes only about one hour. The printing process itself then takes approximately 24 hours, followed by about half an hour of post-processing such as support removal and sanding. In contrast, traditional methods not only rely more heavily on manual labor, but the entire delivery cycle often spans several weeks.
3D printing is transforming rehabilitation orthotics—and this is happening right now.

According to reports, well-known 3D printing content creator “Owen来造” (Owen to Make) has been closely following related projects and released a video titled “How 3D Printing is Transforming a Traditional Industry: Rehabilitation Orthotics.” According to the video, after some orthotic clinics introduced 3D printing solutions, they completed over a hundred patient cases in just six months, with approximately 80% of patients actively choosing this type of orthotic device.
Based on current clinical feedback, the short-term difference in corrective effectiveness between 3D-printed orthotics and traditional ones is not significant. However, in the long run, the improved wearing experience is likely to enhance patient compliance, thereby widening the gap in overall treatment outcomes.
The Real Bottleneck Lies in Materials
That said, the story is not without its challenges.
In recent years, 3D-printed rehabilitation orthotics have relied heavily on technologies such as MJF (Multi Jet Fusion) and SLS (Selective Laser Sintering), typically using nylon materials. These methods offer good forming quality and mechanical performance, but the costs remain persistently high.

In contrast, the technology with true potential for large-scale adoption is FDM (Fused Deposition Modeling), which is more widely available and significantly lower in cost. However, material performance has long been the core limiting factor—issues such as insufficient interlayer adhesion, weak mechanical properties in the Z-axis direction, and limited long-term reliability have restricted its further penetration into the rehabilitation orthotics field.
Breaking Through from the Materials Side
For example, Polymaker, a 3D printing materials manufacturer, has introduced OrthoTough 1000—a material specifically optimized for orthotic bracing applications.

According to publicly available data, it can withstand 100,000 open-close cycles without deformation and 30,000 bending cycles without breaking, with significantly improved impact resistance in the Z-axis direction. At the same time, its strength is close to that of traditional PP (polypropylene), without fully sacrificing toughness.

More importantly, materials of this type have already passed biocompatibility tests such as GB16886 and ISO10993, and have entered the medical device registration system. For 3D-printed rehabilitation orthotics, this means the most critical barrier—materials—is gradually being overcome.
Change Has Already Happened—It’s Just Not Over Yet
If we only look at the outcome, 3D printing has not yet completely replaced traditional orthotics. But if we look at the process, the industry has already shifted to an entirely new logic.
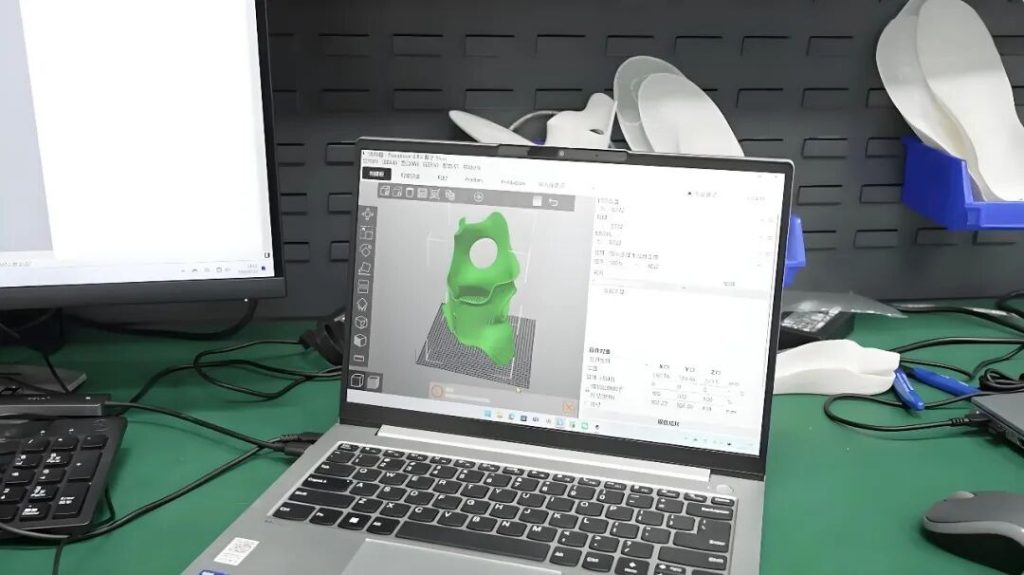
Design is shifting from experience-driven to data-driven; manufacturing is moving from manual craftsmanship to digital production; products are evolving from single-function orientation to a balance of experience and personalization; and production is gradually transitioning from one-off customization to mass customization. At the same time, more subtle changes are also taking place: patient data can be stored and reused, damaged orthotics can be quickly reproduced, and the entire manufacturing process has become cleaner and more efficient.
These changes may not explode in the short term, but they will continue to accumulate.
Once materials and costs cross the critical threshold, this long-undervalued rehabilitation orthotics market will most likely be redefined by 3D printing.
